Margaret Jasinski is an Account Manager for Phigenics. She oversees accounts within the Central Florida region and creates comprehensive water management programs for her clients. Margaret enjoys discussions about public health strategies, health reform and policy, and mindful leadership.
Margaret Jasinski is an Account Manager for Phigenics. She oversees accounts within the Central Florida region and creates comprehensive water management programs for her clients. Margaret enjoys discussions about public health strategies, health reform and policy, and mindful leadership.
As Public Health Professionals, it is imperative to engage with our hospital communities to ensure patient safety goals are being met at the highest standards and with best practices. The leaders at the forefront of driving this culture within healthcare are most likely Infection Preventionists (IPs), which in the past were referred to as Infection Control Professionals. The terminology shift from “control” to “prevention” indicates how this profession has evolved, and how now, more than ever, prevention aligns with proactivity and defensibility. This paradigm shift is further supported by the APIC Competency Model for Infection Preventionists, which is composed of three main pillars - Leadership and Program Management, Infection Prevention & Control, and Performance Improvement and Implementation - all related through program planning, active surveillance, monitoring, verification and validation of any patient-centered wellness initiative.
.jpg?width=433&name=0%20(1).jpg) The recent Florida Professionals in Infection Control conference highlighted the IP roadmap and importance of IP involvement in infection prevention and risk management within hospital settings for all patients and all risks. Additionally, the Joint Commission published the 2018 National Patient Safety Goals for Ambulatory Health Care to underscore the importance of protecting the most vulnerable of populations, which applies to most in-patients within acute care settings. All of these messages reinforce the notions that patients lean on hospital care to include, but not be limited to, the following: safe environment, caring network of staff, and exceptional care to mitigate any and all health ailments. With these expectations comes the obligation to ensure a safe and comfortable environment where patients can recover effectively and leave the hospital healthier and stronger than when they arrived.
The recent Florida Professionals in Infection Control conference highlighted the IP roadmap and importance of IP involvement in infection prevention and risk management within hospital settings for all patients and all risks. Additionally, the Joint Commission published the 2018 National Patient Safety Goals for Ambulatory Health Care to underscore the importance of protecting the most vulnerable of populations, which applies to most in-patients within acute care settings. All of these messages reinforce the notions that patients lean on hospital care to include, but not be limited to, the following: safe environment, caring network of staff, and exceptional care to mitigate any and all health ailments. With these expectations comes the obligation to ensure a safe and comfortable environment where patients can recover effectively and leave the hospital healthier and stronger than when they arrived.
Sometimes forgotten and often mismanaged is the building water system, which poses an environmental safety threat to any recovering patient. With the recent revision of the CMS Memo as well as the newly revised ANSI/ASHRAE Standard 188-2018, Legionellosis: Risk Management for Building Water Systems, it is clear that the core of this effort needs to be driven by the Infection Preventionist on site.
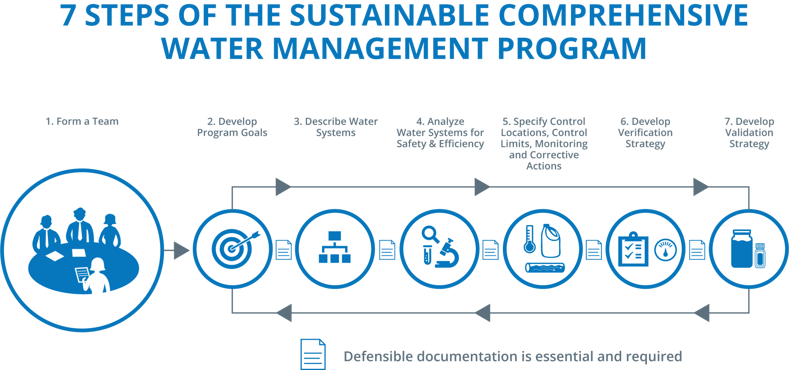
First, their expertise and clinical perspective are necessary to effectively characterize the risk across the hospital facility and identify critical and vulnerable patient populations. Second, the IP is able to support the process of analyzing water systems for safety and assisting in the specification of control locations, critical limits, monitoring activities and corrective actions. Finally, having a clinician on-board for these processes allows for effective and comprehensive cross-communication between Infection Prevention, Engineering, Facilities, Environmental Services and other Water Management Team members as it relates to the prevention of legionellosis and other waterborne pathogens within the hospital water system.
With due diligence and by “doing the right thing,” implementing and maintaining an active Water Management Program at your facility helps protect your patients, guests and staff from any disease-causing waterborne pathogens. As International Infection Prevention Week (October 14-20) approaches, now is the time to take action and get involved with your hospital's water safety program as the theme this year states, “Infection Prevention is Everybody’s Business”. Events like these raise awareness of the key role that infection prevention plays to improve patient safety. We all know awareness is the first step and with intention, the appropriate action will more importantly follow!
.jpg?width=600&name=0%20(3).jpg)